VASA PREVIA, Nathan Fox, MD (Digital)
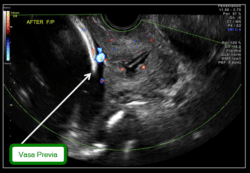
Vasa previa is a rare, but extremely dangerous (to the fetus), condition of pregnancy where a placental blood vessel crosses over the maternal cervix. If not diagnosed, the risk of fetal death is approximately 50%.
The blood vessels in the umbilical cord and inner surface of the placenta are all an extension of the fetal blood circulatory system. Usually, the blood vessels in the umbilical cord enter directly into the middle of the placenta. Sometimes, however, the vessels first travel along the thin placental membranes before entering the placenta. If these membranes are also overlying the cervix, when the woman goes into labor and ruptures those membranes (commonly called “breaking her water”), the blood vessel could burst, causing fetal bleeding. Since the total blood volume of a term fetus is only approximately the same as a can of soda, any fetal bleeding can be catastrophic to the fetus.
The estimated incidence of vasa previa is 1 in 2500 deliveries. There are certain risk factors for this condition, including a placenta previa (where the placenta itself covers the cervix) early in pregnancy that resolves (migrates away from the cervix).
The best way to diagnose vasa previa is with transvaginal ultrasound combined with color Doppler (show in the image above). If diagnosed, patients are advised to have a cesarean delivery prior to the onset of labor, usually at approximately 35 weeks. Frequently, hospital admission is recommended 1-2 weeks prior to delivery to look closely for signs of labor and to be able to respond rapidly if labor or rupture of membranes occur.
Fortunately, in the setting of a known vasa previa, with the above management, the fetal survival is better than 97%. For this reason, the most important aspect of managing vasa previa is diagnosing it!
Maternal Fetal Medicine blogs are intended for educational purposes only and do not replace certified professional care. Medical conditions vary and change frequently. Please ask your doctor any questions you may have regarding your condition to receive a proper diagnosis or risk analysis. Thank you!







