UNDERSTANDING TWIN-TWIN TRANSFUSION SYSTEM (TTTS), Nathan Fox, MD (Digital)
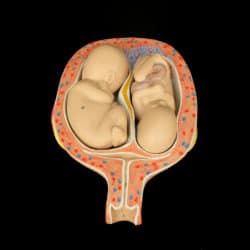
Twin-twin transfusion syndrome (TTTS) is identified when blood flows unequally between monochorionic twins or twins that develop in the same placenta. This condition occurs in about 10 to 15 percent of monochorionic twin pregnancies. There is no concrete evidence of the development or genetic causes of TTTS.
Symptoms of Twin-Twin Transfusion Syndrome
Twin-twin transfusion syndrome has an unequal sharing of blood between twins through the blood vessel connections in the placenta. One twin (the donor twin) provides the other with blood (the recipient twin), which causes the donor twin to receive an inadequate amount of blood and the recipient twin too much blood.
This increased amount of blood leads to the recipient twin leads to a higher production of urine, resulting in too much amniotic fluid (polyhydramnios), and hydrops, which is a prenatal form of heart failure. Conversely, the donor twin produces less urine, which leads to low or no amniotic fluid surrounding it, also known as oligohydramnios. Without medical attention, TTTS can be fatal for the twins.
Diagnosis of TTTS
The primary characteristic of TTTS is whether the twins share a placenta, which is distinguished early on during pregnancy through ultrasound. Other characteristics may include different sized twins, same-sex twins, and a distinct difference in the amount of amniotic fluid around the two fetuses. TTTS can also have a significant impact on the twins’ cardiovascular system, so it’s vital that twins are thoroughly evaluated for heart problems.
A twin-twin transfusion syndrome evaluation may include the following exams:
- Ultrasound – An ultrasound can help rule out development abnormalities. It also analyzes the blood flow patterns in the separate blood vessels for each twin.
- Fetal Echocardiogram – A specific ultrasound that assesses the heart of each twin is important when diagnosing TTTS. This condition may lead to serious cardiovascular complications, such as a serious train in the recipient twin, resulting in an enlargement of the heart.
- Genetic Amniocentesis – If the earlier tests are leading to a diagnosis of TTTS, a procedure may be performed that tests a small amount of amniotic fluid from the sacs around the fetuses. This genetic test is necessary if the ultrasound tests find structural malformations.
Based on your test results, you and your doctor will discuss treatment options based on the stage of your twin-twin transfusion syndrome.
Treatment of TTTS
There are various management options for women diagnosed with twin-twin transfusion syndrome, including:
- Fetoscopic Selective Laser Ablation – This minimally invasive procedure is performed on the placenta to disconnect the twins blood vessels. It essentially halts the sharing of blood from the twins, which stops the progression of TTTS. This is generally the preferred treatment for TTTS, based on the placenta location, stage of TTTS, and gestational age.
- Fetal Monitoring – If no surgery is recommended, close monitoring using intermittent ultrasound tests to evaluate the condition of the twins is helpful in expectant management. It’s important to look for signs of progression. If there are any changes, a follow-up fetal echocardiogram is recommended to ensure a healthy outcome.
- Amnioreduction – This surgical intervention involves the removal of unnecessary amniotic fluid from the recipient twin, which can improve discomfort that the mother experiences from fluid buildup. However, this treatment option is temporary and may need to be repeated.
- Selective Cord Occlusion – Another minimally invasive surgery that stops blood flow to one twin to improve the outcome for the other twin. This procedure involves bipolar cord coagulation and radiofrequency ablation. This is generally considered the last option for expecting mothers who are at an advanced stage of TTTS and the at-risk twin is not likely to survive.
If you undergo medical intervention due to TTTS, your doctor and care team will help provide post-operative instructions. It’s also necessary to have a follow-up appointment to reevaluate the health of your twins. Ultrasound exams will then be scheduled accordingly based on your doctor’s recommendations for the duration of the pregnancy. For more information, visit our blog page or contract us.
Maternal Fetal Medicine blogs are intended for educational purposes only and do not replace certified professional care. Medical conditions vary and change frequently. Please ask your doctor any questions you may have regarding your condition to receive a proper diagnosis or risk analysis. Thank you!







