PAIN RELIEF OF LABOR AND DELIVERY, Michael Silverstein, MD (Digital)
There are five methods most commonly used as methods of pain relief used on labor and delivery. These include epidural, spinal and local anesthesia, IV sedation, and general anesthesia. Today we will discuss spinal anesthesia.
What is Spinal Anesthesia?
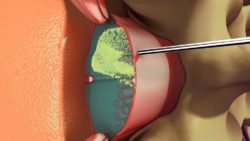
Anatomically, the path between the skin of the back and the spinal cord crosses skin, subcutaneous tissue, cartilage that separates the discs, ligament, and the dura (the sheath that houses the spinal fluid and spinal cord). Spinal anesthesia involves injecting medications beyond the dura to allow mixing with the spinal fluid at a level below which the spinal cord ends.
Spinal anesthesia is similar to an epidural, but its effects are felt faster since it is administered into the spinal canal. We use spinal anesthesia for the majority of our scheduled cesareans, due to the rapid onset of pain relief, as well as the short action (3-4 hours) of the medications. It involves a single injection, and no catheter is needed.
For cesarean patients, a second medication is included in the spinal anesthesia; a milder longer-acting (18-24 hours) medication then reduces the need for pain medications in the first several hours after the surgery.
The History of Spinal Anesthesia
Spinal methods were initially used in the late 1800s, with cocaine as the only choice of medication, but became unpopular due to the toxicity of this medication. As safer medications were developed, spinal anesthesia became more and more popular. Due to its inhibition of movement, it was largely replaced by epidural for laboring patients.
Who Can Receive Spinal Anesthesia?
Women who undergo cesareans commonly receive spinal anesthesia. However, those with abnormally low blood pressure, a bleeding disorder, or a blood or skin infection, or those who have had a previous allergic reaction to local anesthetics should not receive this form of anesthesia.
Learn More on the Healthful Woman Podcast
Maternal Fetal Medicine blogs are intended for educational purposes only and do not replace certified professional care. Medical conditions vary and change frequently. Please ask your doctor any questions you may have regarding your condition to receive a proper diagnosis or risk analysis. Thank you!







