WHAT ARE THE EFFECTS OF ANEMIA IN PREGNANCY?, Andrei Rebarber, MD (Digital)
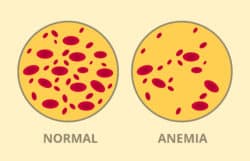
Anemia is a medical condition in which your blood does not contain enough healthy red blood cells or hemoglobin. These red blood cells and hemoglobin help to bind the oxygen, then transporting oxygen to cells throughout the body. Pregnant women are particularly susceptible to developing anemia since they are producing more blood to support the growing fetus. In addition to this, an iron deficiency would also affect one’s ability to produce a suitable amount of red blood cells.
According to the Centers for Disease Control and Prevention (CDC), they have defined anemia in pregnancy as hemoglobin levels of less than 11 g/dL in the first and third trimesters and less than 10.5 g/dL in the second trimester. It is reported that 16 to 29 percent of pregnant women in the United States become anemic in the third trimester, and women with twins are at increased risk of developing anemia.
What are the Effects of Anemia in Pregnancy
The adverse maternal and fetal effects of iron deficiency anemia in pregnancy were illustrated in a retrospective review of 75,660 term single baby deliveries at a single institution, 11 percent were associated with maternal iron deficiency anemia at the time of delivery. Compared with controls, women with iron deficiency anemia were at increased risk of requiring a transfusion, preterm delivery or cesarean delivery. Increased adverse fetal outcomes included 5-minute Apgar, intensive care admission, macrosomia (high birth weight) and large for gestational age. Anemic women were also more likely to be younger and carrying multiples.
How is it Treated?
First, we look to treat our patients using oral supplementation of iron to improve maternal blood counts and increase iron stores; however, we can use intravenous iron to treat iron deficiency anemia in pregnant women in conjunction with a hematologist for those resistant to oral therapy. The efficacy of this approach was demonstrated in a series of 189 consecutive pregnant women with hemoglobin levels less than 10.5 g/dL who were treated with 1000 mg of IV iron during the second or third trimester of pregnancy in singleton gestations with improved blood counts.
Maternal Fetal Medicine blogs are intended for educational purposes only and do not replace certified professional care. Medical conditions vary and change frequently. Please ask your doctor any questions you may have regarding your condition to receive a proper diagnosis or risk analysis. Thank you!







