UTERINE ANOMALIES AND ASSOCIATED CAUSES, Nathan Fox, MD (Digital)
Congenital abnormalities of the uterus, or congenital müllerian anomalies, are malformations of the uterus that develop during the embryonic stage of fetal growth. Some examples of these anomalies include uterus didelphys, arcuate uterus, unicornuate uterus, bicornuate uterus, and septate uterus. When an individual is in their mother’s womb, the uterus begins to form in two separate halves. These two tube-shaped structures, called the müllerian ducts, later fuse together to create one uterus. For some, the connection of these two ducts is incomplete, or fuses in a way that results in an abnormal uterus. These anomalies are often asymptomatic and go unrecognized for the majority of a woman’s early life. A woman’s medical history and physical exam findings may cause an obstetrician to suspect a uterine anomaly, but an ultrasound or MRI is required to confirm a congenital uterine anomaly diagnosis. The prevalence of uterine anomalies has been reported in approximately 2-4% of reproductive-age women, and in up to 5-25% of women who experience complications regarding pregnancy outcomes. It is possible to have no physical or reproductive symptoms of an abnormal uterus making the true number of women with uterine anomalies unknown, as screening for uterine anomalies is typically only performed when a woman experiences abnormal gynecological symptoms or has repeated adverse reproductive outcomes.
Types of Uterine Anomalies
In most cases, the classification of uterine anomalies follows the 1988 American Fertility Society classification of müllerian anomalies and includes uterine hypoplasia/agenesis, unicornuate uterus, didelphys uterus, bicornuate uterus, septate uterus, arcuate uterus, and DES drug-related. In some instances, uterine anomalies fall between two categories and are classified as hybrid or complex. Nonsurgical diagnosis of uterine anomalies can be made by ultrasound, MRI, or hysterosalpingogram. Saline-infusion-sonohysterogram (SIS), an imaging procedure in which a wand that releases sound waves is inserted into the vagina while a small catheter releases sterile saline in the uterus in order to record and map the structure of the uterus, is a highly reliable diagnostic procedure with over 95% accuracy.
Among congenital uterine anomalies, the following are the most common:
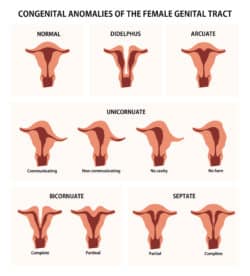
- Arcuate: A minor irregularity in the shape of the uterus, causing a small dent in the top.
- Septate: The uterus is divided by a band of muscle or tissue creating two separate cavities within the uterus.
- Bicornate: Similar to a septate uterus, a bicornate uterus also known as “heart-shaped,” has two cavities created by a wall of tissue, but also has an external fundal indentation of more than 1cm.
- Didelphys: Additionally known as a “double uterus”, women with this rare abnormality have two separate uteruses with smaller cavities than a normal uterus. Each uterus has its own cervix, fallopian tube, and ovary.
- Unicornuate: This abnormality is classified by only one half of the uterus developing, resulting in only one fallopian tube.
- Retroverted or Tipped Uterus: It is important to note that this is not considered an abnormality, but a uterine variant similar to being left-handed vs right-handed. A retroverted uterus tips backward and is seen in about 20-25% of women. It does not typically cause any gynecologic or pregnancy complications, but a small percentage may have increased pain during the beginning of pregnancy due to the growing uterus pushing up against the sacral bone. In rare occasions, the uterus can get “stuck” and needs to be manipulated by a doctor so that it may grow out of the pelvis.
Associated Complications
The presence of a uterine anomaly appears to increase the risk of adverse pregnancy outcomes. Adverse pregnancy outcomes, sometimes called adverse reproductive outcomes, include miscarriage, preterm birth, fetal growth restriction, malposition, cesarean delivery, and preeclampsia. Certain anomalies pose a greater risk for some of these complications than others. An association between uterine anomalies and renal (kidney) anomalies has also been identified as they have related embryologic precursors (cells that later develop into certain organs).
Treatment for Women with Uterine Abnormalities
Women with uterine abnormalities should be closely supervised in pregnancy due to their increased risk of complications. Such complications could include premature birth or diminished fetal growth during pregnancy. Women with a septate uterus may have an increased risk of early miscarriage if the pregnancy spontaneously implants onto the septum itself, instead of on the uterine wall. Women with uterine abnormalities may also be more likely to have babies in the breech position during labor or require a c-section. Your obstetrician or maternal fetal medicine specialist will inform you of what you can expect throughout the duration of your pregnancy and labor.
In some cases, the uterus can be repaired with surgery. For example, those with a septate uterus may opt to undergo surgery to remove the wall of tissue separating the uterus thus reducing the risk of miscarriage. This is not a guaranteed solution but does show great potential in leading to successful pregnancies.
Because uterus development and kidney development have related embryologic precursors women with uterine abnormalities should have their kidneys checked, usually with an ultrasound, to ensure they are both normal appearing. This, in addition to evaluating risks related to pregnancy, can allow those with a uterine abnormality to modify their expectations and identify a course of action that can help them live a normal life.
Maternal Fetal Medicine blogs are intended for educational purposes only and do not replace certified professional care. Medical conditions vary and change frequently. Please ask your doctor any questions you may have regarding your condition to receive a proper diagnosis or risk analysis. Thank you!







