PAIN RELIEF ON LABOR AND DELIVER: EPIDURAL, Michael Silverstein, MD (Digital)
The five most commonly used methods of pain relief used during labor and delivery are spinal anesthesia, epidurals, local anesthesia, IV sedation, and general anesthesia. Today we will discuss epidural anesthesia.
What is Epidural Anesthesia?
Epidural anesthesia is the most popular type of pain relief used during labor. In fact, 60-90% of women who give birth use an epidural. It is a form of regional anesthesia, meaning that is blocks pain in certain areas of the body. The main goal of an epidural is the provide pain relief by blocking the nerve signals from the lower spine. This results in a numbing sensation in the lower half of the body.
The dosing of an epidural is patient-driven. For example, if you are too numb, we allow the dose to fall; if you are too uncomfortable you will have a button to increase the level. In addition, the OB Anesthesia team is on the labor floor 24-7 to assist.
If you need an operative vaginal delivery or a cesarean section, the level of pain relief can be adjusted to allow these procedures.
How is an Epidural Administered?
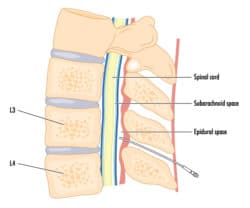
An epidural is administered by an anesthesiologist or nurse anesthetist before active labor begins. Patients will be asked to lie on their side or sit up, arch their back, and remain still. A small area of the lower back near the spinal cord will then be injected with local anesthetic to numbed the area. A needle is then inserted into the numbed area. Then, a small tube or catheter will be threaded through the needle into the epidural area. The needle will be removed, leaving the catheter in place to provide medication.
The History of Epidural Anesthesia
Epidurals (as a single injection) were initially used in the early 1900’s as an alternative to spinal or inhaled anesthesia. In the 1930’s, the first catheter was used, allowing continuous administration. In the 1970’s, epidurals became quite popular. Currently, anywhere from 60-90% of laboring patients request and receive epidurals.
Is Epidural Anesthesia Safe?
Yes; there is no evidence that epidurals prolong labor, increase the rate of cesarean sections, or have any detrimental effect on the newborn.
Our practice recommends you keep an open mind; if you arrive in active labor and the birth appears to be only a few hours away, you may prefer not to have an epidural. If you arrive in early labor and the birth does not seem to be imminent, you may prefer to receive an epidural.
Learn More on the Healthful Woman Podcst
Maternal Fetal Medicine blogs are intended for educational purposes only and do not replace certified professional care. Medical conditions vary and change frequently. Please ask your doctor any questions you may have regarding your condition to receive a proper diagnosis or risk analysis. Thank you!







